Your Guide To Better Mental Health And Relationships.
The Minds Journal is a mental and emotional wellness platform which encourages individuals to improve their mental and emotional health by offering a wide range of high-quality resources like –
- Informative articles
- Heart-touching blogs
- Inspiring quotes & thoughts
- Reader-submitted real-life stories
- Psychological & Self-awareness tests
- Motivational videos
Our resources are designed to help people develop positive thinking and convert it into positive action by making informed decisions.
The Minds Journal Collection
Toxic Love Disorder: Your comprehensive guide to understanding, overcoming, and healing from toxic relationships.
EXPLORE OUR ARTICLES
Sort Articles By Genre
Find passionately crafted blogs and articles written by expert authors on different topics.
Didn’t find what you need?
FEATURED ARTICLES
Latest Blogs & Articles
Explore our latest blogs and articles on a wide range of topics freshly cooked by our team of expert authors from around the globe.
Latest News & Horoscope
QUOTES THAT INSPIRE
Sort Quotes By Genre
Explore quotes that don’t just motivate, but celebrate love, heartbreak, pain and the human spirit.
Didn’t find what you need?
WORDS OF WISDOM
Latest Collection Of Meaningful
Quotes
Get inspired to live an elevated life with these deep, touching quotes from philosophers, warriors and authors.
Reader Submitted CONTENT
Our Reader’s Blog
Hand-picked blogs, articles, thoughts and poems submitted by our readers and followers.
Didn’t find what you need?
ENTERTAINMENT AND FUN
Quiz & Zodiac
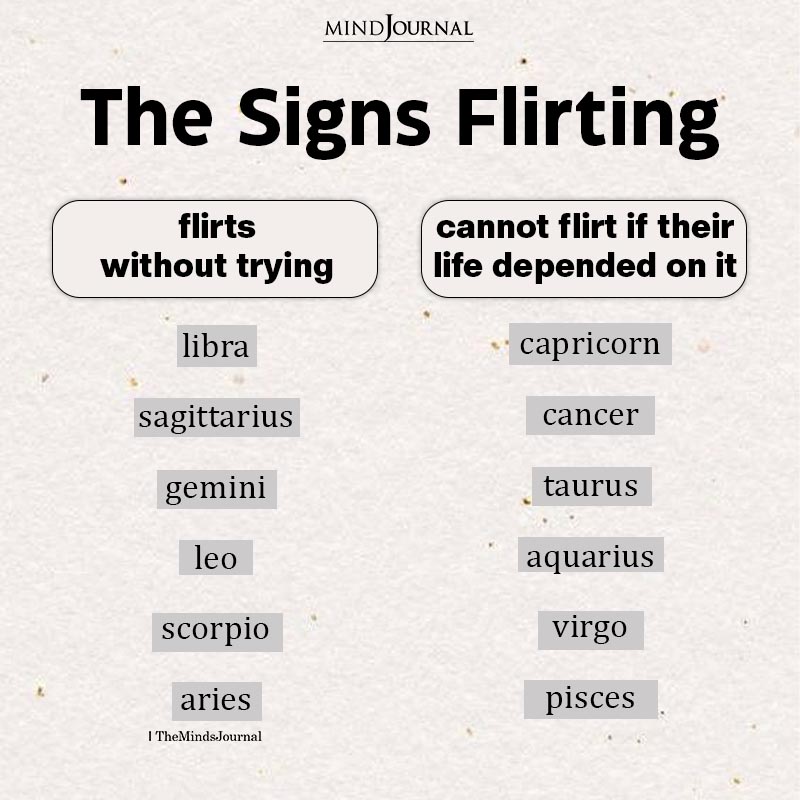
Fun and exciting articles on horoscope, zodiac, personality tests and quizzes that inform and entertain at the same time.

Mind Journal Community
Minds Journal is the largest, independent & free, multi-platform, supportive global community on mental and emotional wellness.
We are determined to start a mental health revolution, to destigmatize mental health issues, and empower people through our self help tools.
Our supportive network ensures people who are suffering feel heard, understood, wanted and connected, not isolated.
Our growing network to spread mental health awareness brings together mental health professionals, writers and readers to share and discuss thoughts & ideas that promote well-being and self-development.
TMJ
MH
WMH
Get advanced Mood Tracker
MENTAL HEALTH TESTS
Self-Assessment On Mind Help
Learn more about your mind, psyche and mental health with our expert verified tests on mental illnesses.
Didn’t find what you need?
Need Mental Health Support?
Mental Health Conditions
1
What Is Good Mental Health?
Good mental health helps us function effectively in daily life, cope with daily life stressors and manage mental health issues positively.
2
Why Is Mental Health Important?
Different psychological conditions can affect various aspects of our life. Taking care of our mental health is crucial for a healthy, productive and happy life.
3
How To Improve Your Mental Health?
If you are struggling with mental health issues, self-help coping strategies like relaxation techniques can help. But the most recommended way is to consult a mental health professional.
4
How Can We Help?
The Minds Journal and Mind Help provides reliable and helpful support through research-backed resources and an unprecedented network of mental health professionals.
Instantly access the best online support and connect with the leading mental health experts from around the globe.